Public records requests show the front-line workers face a perilous funding cliff.
Virginia is set to lose about 60 Community Health Workers employed at local health districts by July 1, 2024.
WMRA and VPM rural health care reporter Henry Brannon reports.
More than 25 additional workers will follow in the year after that. There are 112 CHWs employed at 25 of Virginia’s 35 health districts as of July 2023.
The revelation comes from internal Virginia Department of Health documents, which name the federal grants that fund the positions and when they end. VPM News/WMRA obtained the documents through public records requests.
Community Health Workers are on-the-ground public health workers who come from within the communities they serve. Their work has been essential in COVID-19 vaccination efforts, opioid-overdose reversal training, STI prevention and many other initiatives in Virginia.
Health department documents show it would cost about $5.7 million to fund all 112 positions for a year. Gov. Glenn Youngkin released his budget for the next two years on Wednesday, which did not include funding for Community Health Workers.
The funding cliff has left health districts scrambling to find money for jobs many districts cite as essential to gains they’ve made since the COVID-19 pandemic.
Lucas Tuning is a certified Community Health Worker in Franklin County. He and colleague LaShara Wade were hired by the United Way of Roanoke Valley in 2021. The positions were funded with money the West Piedmont Health District got from a U.S. Centers for Disease Control and Prevention grant.
The pair was quickly tasked with getting the county, especially its Black residents, vaccinated with the then-newly released COVID-19 vaccine.
“Initially, LaShara and I, we got together and we said, ‘OK, how are we going to do this?’” he said.
They knew they had to fight long-standing mistrust of public health institutions that many Black residents felt, Tuning said. Because the population of the area is older, (at 64, Tuning said he’s considered “young folk” at his church) events like the 1932 Tuskegee Syphilis Study are not abstract entries in a history book.
Instead, the decadeslong study — where nearly 400 Black men weren’t told they had syphilis by government health institutions and were monitored, but not treated — remains a concrete memory in the minds of Franklin County’s older population.
Tuning and Wade agreed the outreach would have to be face-to-face to battle that mistrust. “We knew, as far as the folks here in Franklin County, I cannot just give you a flyer and say, ‘Read this,’” Tuning said. “There had to be a face-to-face conversation.”
The next issue was how to reach a substantial number of people while maintaining that face-to-face approach.
“I can't make any kind of ground doing a one-on-one,” Tuning said. So he looked to the Pigg River Community Center, headquarters for about 20 Black churches in the area as well as service providers like Tuning.
Speaking to VPM News/WMRA from the center, Tuning said, “They have fifth Sunday services here. So I talked to one of the ministers. … I said, ‘Look, Reverend, can I get on the program when you're doing announcements and what have you and talk about what we need to do as a community?’”
Once he had the reverend’s buy-in, Tuning got in front of the church congregations and made the case for getting vaccinated. He started by acknowledging Tuskegee and the contentious politics of the vaccine. Then he made two arguments.
“I gave them the positive reason why,” he said. "You want to be here, you want to make sure you protect your family, protect your neighbors."
And he shared a harsher picture, too.
"So what is it going to look like for you, your family members when they're planning your funeral here at the local funeral home?” Tuning told them. “Because today we're having a church service. Next time we're looking at you, we could be having your funeral in this building."
The speech was a success. “The phones was ringing off the hook,” he said. “It was close to 400 folks that we had that had signed up for the vaccine.” Tuning and Wade also set up a drive-thru vaccination clinic at the local disability nonprofit his wife runs.
I'd be willing to sacrifice my job if it bought more community health workers, because what they're doing is more important than what I'm doing. Nancy Bell, population health manager at West Piedmont Health District
And work like this has paid off in the rural county of about 55,000 people.
While the white population of Franklin County was vaccinated for COVID-19 within the last year at slightly higher rates than the Black population (7.3% versus 6.1%), the disparity between those rates is much smaller in Franklin County than in Virginia at large (12.5% versus 7.8%), according to Virginia Department of Health data.
Tuning said the success stemmed from the trust people had in him because of his relationships within the community.
For starters, he was born in the area and, except for the 20 years he served in the military, he’s lived there his whole life. His late mom, Sadie Tuning, was a respected town councilor in nearby Rocky Mount during the 2000s.
Tuning said people hear him out more than they might otherwise when he tells them who his mom was. And many Black community members also appreciate his work bridging gaps between their community and the health department.
“I've had so many members of the community that say that they appreciate having someone that looks like them in the system working with the Health Department,” he said, adding that some told him they wouldn't otherwise have trusted the vaccine.
Tuning and Wade’s jobs are funded by federal grants from the CDC and the American Rescue Plan Act set to end on June 30, 2024. Tuning said he’s fortunate to have employers see the work as indispensable; the United Way of Roanoke Valley has funded both positions itself for another fiscal year.
But for many of Virginia’s CHWs in other health districts, the situation is even more dire.
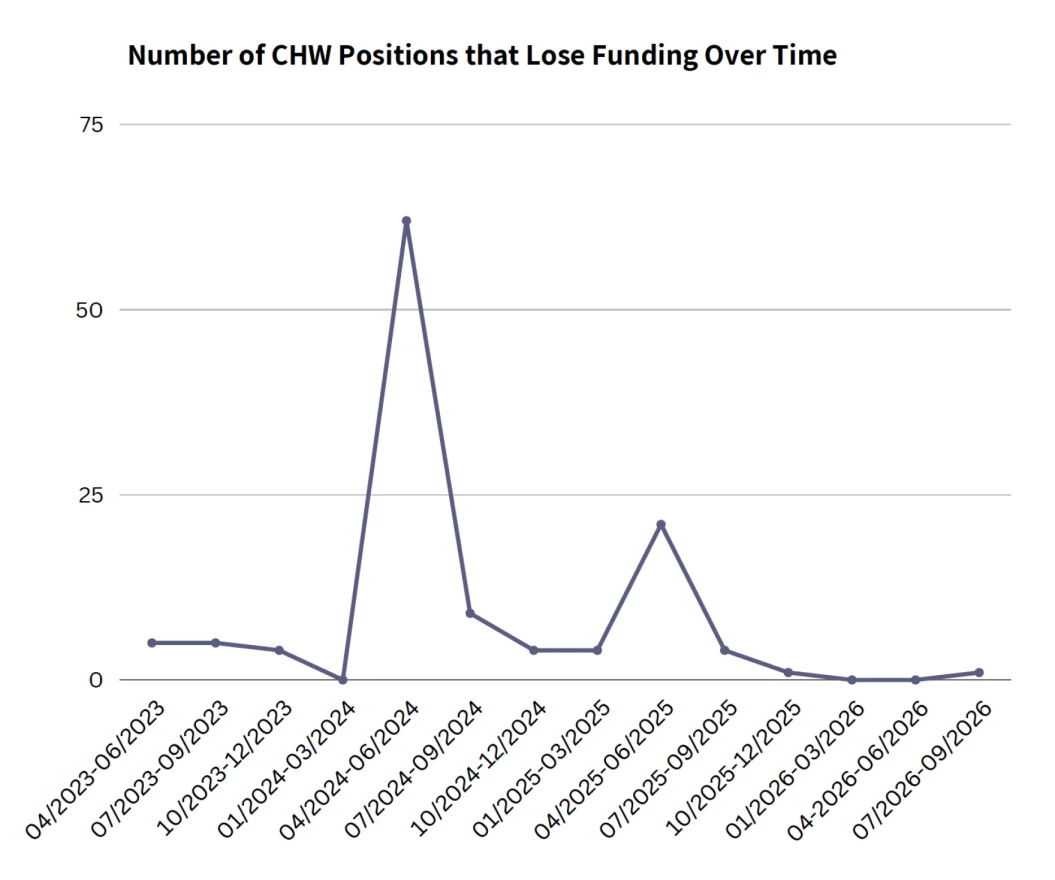
The documents VPM News/WMRA analyzed showed funding for about 60 of the 112 known CHW positions at Virginia’s local health districts will end on June 30, 2024.
About another 20 positions will run out of funding between July 1, 2024, and June 30, 2025. But that data only included 25 of the 35 local health districts in Virginia.
That means there may be more CHWs impacted — though it might not be readily apparent to the public until that money runs out.
According to the documents and more than a dozen people VPM News/WMRA talked to, the worst-case results of this funding cliff will be devastating. Many health districts reported they will no longer be able to operate crucial public health programs — including training on how to use opioid overdose-reversing medication naloxone, community engagement and blood pressure monitoring.
One internal health department document reported 96% of Virginia health districts “strongly agree that loss of funding for CHWs will negatively impact one or more health department programs or services in their health district.” Twenty-five of Virginia’s 35 health districts participated in the survey.
The Virginia Department of Health provided VPM News/WMRA with the following comment: “VDH values the Community Health Worker positions, and we look for continued options for sustainability. The Office of Community Health Services reviewed your inquiries, and a significant amount of time and effort are required to track down all the answers because the questions are complex and detailed. VDH has provided you with some information concerning this general topic in response to your recent FOIA request.”
Youngkin’s office did not respond to VPM News/WMRA’s request for comment on why funding was not included in the proposed budget.
The roughly $175 billion two-year operating budget he presented Wednesday includes a record-high $2.2 billion in funding for the Department of Health.
It would cost about $11.3 million — or 0.5% of VDH’s overall proposed budget — to fund the entire CHW workforce for two years, according to VPM News/WMRA analysis. In a fact sheet, the Virginia Interfaith Center for Public Policy found that number could be reduced to as low as $6 million for the two years.
The average pay for a CHW employed by one of Virginia’s local health districts was $50,141 as of July 24, 2023, according to the documents.

Where CHWs fit in Virginia’s health system
Maybe no one is more sold on the importance of CHWs’ work than Tuning’s boss, Nancy Bell. She’s the population health manager at the West Piedmont Health District in Martinsville, lodged between Southwest and Southside Virginia.
“I'd be willing to sacrifice my job if it bought more community health workers, because what they're doing is more important than what I'm doing,” Bell said. “I don't want people to lose their jobs in public health, but I think community health work is where it's at — and we need to be lifting that up because it really works.”
From district to district, CHWs may operate differently. But the near-universal pattern of their work is filling community needs that would otherwise be neglected.
West Piedmont’s seven CHWs have come to fill a variety of gaps that existed before the COVID-19-era grants that fund their jobs. They provide support for food security, seniors’ needs, COVID-19, housing security and emergency medical services.
“All of the grants that I've gotten since COVID hit, we have made it work for CHWs. Even opioids money, we have peer support Community Health Workers,” said Bell.
In the Central Shenandoah Health District, Population Health Manager Laura Lee Wight told VPM News/WMRA the district’s program started with fighting COVID-19 but grew to other essential areas. Those include food and housing security like West Piedmont’s team, but also navigating complex state and federal programs like Medicare and Medicaid.
Wight said that some of their most important work is bridging gaps between Latino communities in the Shenandoah Valley and the local health department.
“Having a connection to a Community Health Worker who speaks your language, has been through what you've been through is really, really critical to being able to achieve better health outcomes,” Wight said. “Because you have somebody there who can be your advocate, especially when you might not speak English.”
Research backs that up. One study out of Chicago found CHWs bridged gaps between academic health researchers and low-income Latinos. Research also shows CHWs can be extremely successful at addressing some of public health’s most persistent problems.
A 2017-18 CHW initiative in Danville aimed at lowering emergency room visits succeeded by between about 20% and 75% for various patient groups.
Over more than a dozen conversations, VPM News/WMRA heard 31 unique stories of the work CHWs provide. Shanteny Jackson, executive director of the Virginia Community Health Worker Association, shared one of them.
When Jackson was a Community Health Worker in the Richmond and Henrico Health District, she met a Spanish-speaking woman who had been taking one of her medications 11 times a day. When Jackson asked the woman why, the woman explained she saw “once” on the discharge information.
Jackson, a native Spanish speaker, immediately knew the woman had mistaken the English word for “one time” with the Spanish word for “11” — both are spelled o-n-c-e. Jackson said she sat with the woman and drew a sun and moon to show, “You could take this either in the morning or in the evening … you don't have to have 11 pills, you just need one.”
You could take this either in the morning or in the evening … you don't have to have 11 pills, you just need one. Shanteny Jackson, former Community Health Worker
VPM News/WMRA also heard stories of what happens without CHWs.
Veronica Espinoza is a CHW in Charlottesville. She described working with a pregnant woman who didn’t speak English. The woman was a recent immigrant and had gone to the emergency room, describing problems she was encountering in her pregnancy.
No one at the emergency room spoke Spanish.
“And they thought because the nurse speaks a little bit of Spanish that it was enough,” Espinoza said. “They sent her to her house and the next morning, earlier morning at 3 or 4 a.m., she had a miscarriage at her home by herself.”
Espinoza met the woman shortly afterward, and she says the woman told her, “Even if I tried to explain to them my symptoms, I feel that they didn't care. I feel that it was because I am a Latinx woman. And I feel the nurse never passed out the right message or what I've been saying to her.”
Not only was the experience traumatizing for the woman who miscarried, but it also damaged the broader Latino immigrant community’s trust in that hospital as word of the incident spread, according to Espinoza.
“That's why I feel it's really important that in every single place they're hiring Community Health Workers,” Espinoza said. “To make sure that community members have a support or partner or advocate person who looks like you, speaks your language, [and can] help you to navigate the system and have a better understanding on how everything works here in this country.”
After enough stories, it becomes clear the impact of losing dozens of CHWs would not just devastate key local health initiatives that seek to bridge gaps into communities that have long been ignored and mistreated by the public health establishment. It would also be a validation of those communities' mistrust of U.S. public health institutions.
Espinoza said the loss of medical providers since the start of COVID-19 has already damaged trust in communities she works with.
“We lost so many people, so many jobs,” she said. “When I ask people why they don't continue with a primary care, and some people tell me the same: because it's another new person there. They may struggle — they didn't trust that person.”
For Bell, the loss of CHWs “would be devastating, because they're not just doing health. They're doing basic life needs,” she said. “I think it would really push things back to pre-pandemic levels, which were not great then.”
Scrambling to find sustainable funding
Health officials, advocates and CHWs have their sights set on two long-term solutions to the funding cliff.
The first is for Virginia to permit the services CHWs provide to be reimbursable through Medicaid. During the 2023 session, the General Assembly funded a study to look into reimbursement. For Haines of the Virginia Interfaith Center for Public Policy, this is one long-term backup plan to grant funding because it functions as a safety net for the more than 20 states that reimburse.
“If the health department were to lose some funding for CHWs, you have the ability to reimburse Medicaid for CHW work,” she said. “So there's at least something sustainable that's out there. Virginia does not have that.”
But what Haines and others would most like to see is a budget amendment that allocates ongoing funding for CHW positions at local health districts.
And this is a possibility. State Sen.–elect Lashrecse Aird is a Democrat representing Senate District 13 in Central Virginia. In a statement, she told VPM News/WMRA that working alongside the Virginia Interfaith Center for Public Policy, she “will prioritize funding CHW positions during the 2024 session.”
But in the meantime, the June 30 funding cliff has left local officials scrambling to find funding to replace the CDC’s COVID-19 Vaccination Supplement Four grant.
Wight of Central Shenandoah Health District said her district is focused on finding multiple sources to fund the CHW program. She said this “braided funding” approach ensures stability and sustainability.
“A realistic approach for us to continuing the program is to identify additional funding, and braiding those grants with local, state and federal funding, working with our stakeholders to continue to identify funds,” she said. “So we are actively doing that.”
Wight said the primary grant that covers the district’s CHWs is not set to expire until June 2025. While she cautioned that funding could run out sooner, the end of one grant does not necessarily mean the end of the program overall.
“I don't want it to come off like [the CHW program is] not available after this date because that isn't necessarily true,” She said. “That's what our current timeline looks like. But I could get a new grant tomorrow that would change that.”
Bell's work in the West Piedmont Health District is proof that’s a real possibility.
“From day one, I knew that it would go away when the grants [ended], and I never want that to happen,” Bell said. “Since day one, I've been trying to get money, funding, support so that when this grant ends, we have something else in place.”
Bell has approached governments, nonprofits and even “private citizens who can write a check for a good cause.” And she’s been successful.
To fund the seven CHWs in her district, she’s used grants from the CDC, the American Rescue Plan Act and the Virginia Rural Health Association. WPHD has also partnered with two local chapters of United Way, the Virginia Harm Reduction Coalition, the Southern Area Agency on Aging and the Henry-Martinsville Coalition for Health & Wellness.
Bell even put $215,000 of the district's marketing funds into the CHW program to support their outreach work.
“All of that because everyone has skin in the game, and everyone can benefit from these Community Health Workers,” she said. “We have just scratched the surface of what they're going to be able to do.”
And she isn’t stopping anytime soon. In fact, Bell has her sights set on the next project: CHW paramedics to counter high rates of infant and maternal mortality in the region’s maternity care deserts.
The Virginia CHW Association is having a Community Health Worker Education and Awareness Day on Thursday, Jan. 18 at the Virginia General Assembly.


